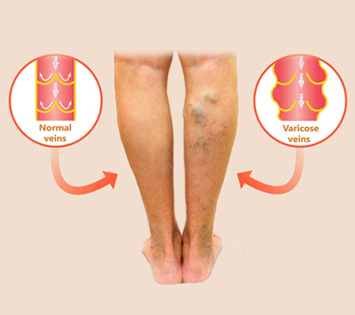
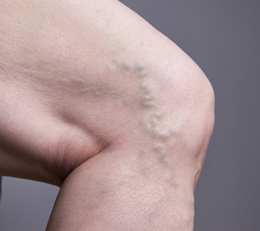
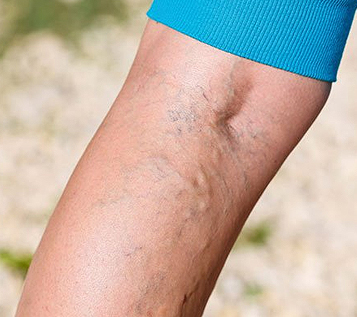
As you age, or in response to disease or injury, the veins in your legs sometimes develop faulty valves that allow the blood traveling to your heart to leak backward into the surrounding tissue. This causes varicose veins, skin ulcerations and swelling, especially in your ankles. These veins can be unsightly and painful when you’re standing.
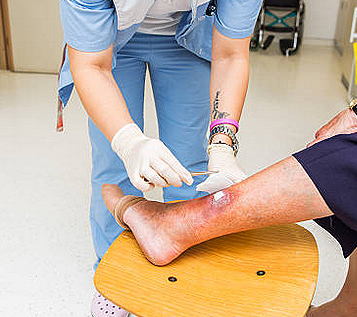
Today’s modern medicine has evolved to make this a successful surgical procedure for removing varicose veins. While many nonsurgical procedures exist and should be considered first, phlebectomy has been proven effective, especially when performed by an experienced vein doctor. It’s primarily performed on larger, superficial veins, so it is not useful in every case.